Approximate Read Time: 13 minutes
ACL rehab programming proves that time alone doesn’t reduce re-injury. Risk completion, criteria, and exposure to real sport demands determine whether athletes truly return ready.
What You Will Learn
- ACL rehab programming succeeds when preparation replaces timelines as the primary decision driver.
- Meeting objective criteria matters more than delaying return-to-sport milestones.
- Incomplete rehab, not early return, explains persistent ACL reinjury rates.
When Waiting Longer Still Isn’t Enough
This past Sunday two notable NFL players tore their ACLs (Patrick Mahomes and Micah Parson). By the time you read this, the headlines will have shifted to already talking about timelines when the players will be back playing.
We are still talking about the same injury in the same way we have for decades, how long it will take to come back, while quietly ignoring the more uncomfortable question: why are we still failing athletes despite longer rehab timelines?
On paper, ACL rehabilitation has evolved. Return-to-play timelines are longer than they were ten years ago. Objective testing is more common. Psychological readiness is at least mentioned now, if not always addressed. And yet, reinjury rates stubbornly refuse to drop. The ACL paradox is this: rehab has become slower, but not safer.
This article is about ACL rehab programming. Not ACL surgery. Not graft choice. Not the highlight-reel injury itself. Programming is the integration between biology and performance.
What Elite-Level Data Actually Shows About ACL Rehab
When we talk about ACL outcomes, recreational data often dominates the conversation. But professional athletes are where systems are most refined, resources are abundant, and margins are smallest. If something is failing there, it matters.
A 2025 systematic review and meta-analysis of nearly 2,000 professional soccer players examined return-to-play outcomes across three eras of ACL reconstruction: 2011–2016, 2017–2021, and 2022–2025 (D’Ambrosi, 2025). The findings are interesting in their consistency and their contradiction.
More than 92% of professional players returned to play. Roughly 80% returned to their pre-injury level. On the surface, those numbers sound reassuring. But dig deeper and the story changes.
The average time to return to play increased by over 40% in the most recent era, rising from roughly 6–7 months to nearly 10 months. This shift reflects what many clinicians believe is progress: more conservative timelines, better respect for graft biology, and greater emphasis on criteria-based decision-making.
But here’s the problem. The graft re-rupture rate did not meaningfully change. Across all eras, it hovered around 8% (D’Ambrosi, 2025).
Slower did not mean safer.
This finding begs us to ask additional questions about these longer timelines. If time alone were protective, we would expect re-injury rates to fall as timelines lengthened. They did not. That forces an uncomfortable conclusion: we are delaying return without fundamentally changing the quality of preparation.

The Myth of the Calendar-Based Comeback
For years, nine months has been treated like a magic number. Wait long enough and risk supposedly drops. And to be clear, biology does matter. Graft ligamentization is not instantaneous. Muscle hypertrophy and strength does not happen quickly.
But the evidence no longer supports time as a stand-alone solution.
A large prospective cohort study of male athletes returning to pivoting sports followed over 500 athletes through rehabilitation and two years post-surgery (Kotsifaki, 2025). The researchers asked a deceptively simple question: does returning before or after nine months change reinjury risk—if athletes actually meet discharge criteria?
The answer may surprise you. Among athletes who completed rehabilitation and met objective discharge criteria, time to return was not associated with re-injury risk (Kotsifaki, 2025). Returning before nine months was not inherently dangerous. Returning unprepared without achieving known criteria is more critical than time alone.
This distinction matters. It reframes ACL rehab away from “waiting it out” and toward earning progression through demonstrated capacity.
Biological timelines are important, but perhaps we swung the pendulum too far in that direction with the magic number 9.
Rehab Completion: The Variable We Rarely Talk About
Here is the most under-discussed finding in modern ACL research: most athletes do not actually complete high-quality rehabilitation.
In the same cohort study, adherence and rehab completion showed a clear dose–response relationship with outcomes. Athletes who met discharge criteria were almost six times more likely to return to their sport. Nearly 90% of those who completed rehab returned to pivoting sports. Among those who stopped early, only about half made it back (Kotsifaki, 2025).
This is not a small effect. It is the difference between a career continuing and quietly ending.
ACL rehab is often described as a protocol, but in reality it is a long exposure to progressively increasing demands. Strength, speed, deceleration, rotation, fatigue, and psychological stress all need to be reintroduced. When rehab stops early—whether due to insurance limits, access issues, motivation, or false reassurance—those exposures never happen.
The athlete may look “cleared.” The system may feel satisfied. But the knee has not been prepared for the chaos of sport.
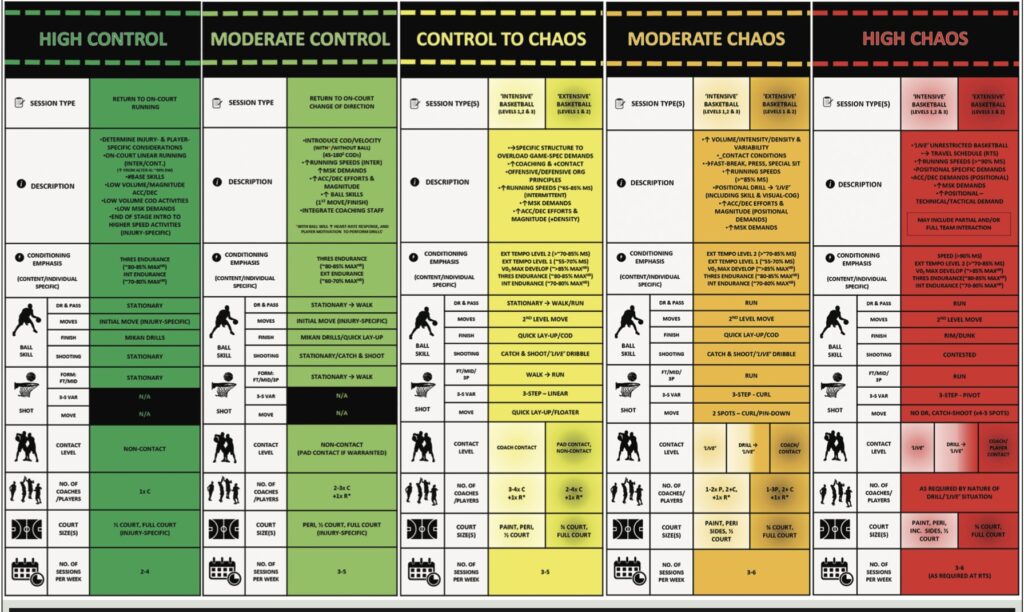
Why Slower Rehab Hasn’t Reduced Re-Injury
If rehab is longer and testing is better, why do reinjuries persist?
Part of the answer lies in what we test—and what we don’t.
The professional soccer meta-analysis highlights several persistent deficits even among athletes who return successfully: quadriceps weakness, altered neuromuscular coordination, and inefficiencies during high-speed, multi-planar movements (D’Ambrosi, 2025). These are not trivial issues. Soccer, football, and basketball all demand repeated deceleration, cutting, and rotational loading that stress the reconstructed graft in ways simple strength tests do not capture.
Think of cartilage or ligament tissue like a construction material. Concrete does not fail because time passed; it fails because load exceeded capacity. ACL grafts behave the same way. If rehab restores strength but not load tolerance under sport-specific conditions, the structure is vulnerable—no matter how long you waited.
Slower rehab without deeper programming is just delayed exposure. And delayed exposure, eventually, still happens.
ACL Rehab Programming vs ACL Rehab Duration
This is where language matters. We talk constantly about how long ACL rehab takes. We also need to talk about what actually happens during that time.
The Aspetar Clinical Practice Guideline on ACL rehabilitation emphasizes this distinction clearly. Rehabilitation should be criteria-based, individualized, and progressive, with time serving as a boundary condition rather than the primary driver (Kotsifaki, 2023). Accelerated timelines can be appropriate when criteria are met. Delayed timelines offer no protection if criteria are ignored.
Programming, in this context, means deliberate sequencing of stress:
- restoring force production,
- re-establishing motor control,
- exposing the athlete to plyometrics and deceleration,
- integrating sport-specific movement,
- and addressing psychological readiness.
Without this structure, time becomes an empty container.
The Hidden Cost of “Successful” Return to Play
Even when athletes return, success is not guaranteed.
Across elite cohorts, approximately 20–25% of athletes never regain their pre-injury performance level (D’Ambrosi, 2025). Some play fewer minutes. Some change positions. Some quietly exit the league.
This drop-off is rarely attributed to rehab quality, but the link is hard to ignore. Persistent strength asymmetries, movement hesitation, and fear of re-injury all shape how an athlete moves once competition resumes.
Setting the Stage for Better ACL Rehab Programming
So where does this leave us?
The evidence no longer supports the idea that waiting longer alone reduces risk. It does support something more demanding: rehab completion, objective criteria, and high-quality programming matter more than the calendar.
In the next section, I’ll break down how modern ACL rehab programming should actually be structured, phase by phase, and why strength symmetry, plyometrics, deceleration, and psychological readiness must be treated as non-negotiables, not optional add-ons.
What Modern ACL Rehab Programming Actually Requires
If time alone doesn’t protect athletes, the obvious follow-up question is what does?
The answer emerging from the last decade of ACL research is not a new exercise, a new graft, or a new device. It’s something far more fundamental and far more difficult to standardize, programming quality across the entire rehabilitation continuum.
ACL rehab is often described as a sequence of phases. In reality, it’s a progressive exposure problem. The knee must relearn how to tolerate force, speed, rotation, uncertainty, and fatigue. When any of those exposures are underdosed—or skipped entirely—the athlete returns with blind spots. Those blind spots don’t announce themselves during clearance testing.
Rehab Is Not a Protocol. It’s a Continuum.
One of the most important conceptual shifts in the Aspetar Clinical Practice Guideline is the rejection of rigid, time-locked protocols (Kotsifaki, 2023). Instead, rehabilitation is framed as a criteria-driven continuum, where progression depends on demonstrated capacity rather than elapsed weeks.
This distinction matters because ACL rehab failures rarely occur early. They occur late when rehab looks “successful” on paper but has not adequately prepared the athlete for sport-specific stress.
The guideline organizes rehab into phases for clarity, but it emphasizes that time is a guardrail, not a driver. You cannot progress too fast for tissue healing, but you can absolutely progress too slowly for performance demands.
Phase 1: Early Rehab Is About Capacity, Not Comfort
The early phase of ACL rehab is often misunderstood. It’s framed as a time to protect the graft, manage swelling, and restore range of motion. All of that is true, but incomplete.
Early rehab is also where voluntary muscle activation is either restored or permanently compromised.
Quadriceps inhibition after ACL reconstruction is not just a short-term inconvenience. Persistent quadriceps weakness has been repeatedly associated with altered movement strategies and increased joint loading later in rehab and after return to sport (D’Ambrosi, 2025).
The Aspetar guideline is explicit here:
- Early unrestricted motion is encouraged.
- Early weight-bearing is safe when controlled.
- Isometric quadriceps activation should begin immediately.
- Immobilization offers no long-term advantage (Kotsifaki, 2023).
This phase sets the ceiling for everything that follows. If the athlete leaves early rehab with incomplete activation or unresolved swelling, every subsequent phase becomes a compensation exercise rather than a performance progression. Blood flow restriction training is a great tool with significant evidence to help mitigate the common setback of muscle atrophy.

Phase 2: Strength Symmetry Is Not a Suggestion
Somewhere in the middle of rehab, many programs quietly change goals. Early on, clinicians fight for every degree of motion and every percentage of strength. Later, the focus subtly shifts toward “doing enough” to move on.
This is where modern ACL rehab often derails.
The Aspetar guideline and recent cohort data are unequivocal: strength symmetry matters (Kotsifaki, 2023; Kotsifaki, 2025). Not because symmetry is aesthetically pleasing, but because asymmetry changes how athletes load the knee during deceleration, cutting, and landing.
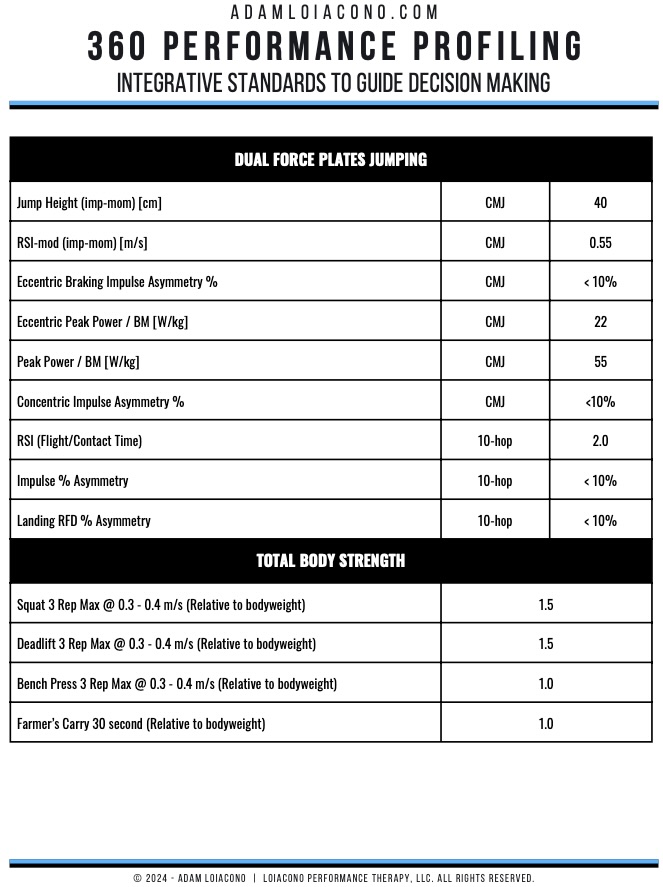
In the male athlete cohort followed by Kotsifaki and colleagues, discharge criteria included:
- 90% limb symmetry for strength
- 90% jump symmetry
- Pain-free testing
- Completion of sport-specific preparation (Kotsifaki, 2025)
Athletes who met these criteria returned at far higher rates and without increased reinjury risk regardless of whether they returned before or after nine months. Strength deficits don’t disappear on their own. The most common place strength deficits will appear is under higher velocities once the athlete begins sport participation.
Phase 3: Running Is Not a Fitness Test, It’s a Load Test
Return to running is often treated like a milestone. In reality, it’s a diagnostic stress test.
The Aspetar guideline notes that most protocols allow running around 12 weeks, but it also highlights the absence of strong evidence tying a specific week count to safety (Kotsifaki, 2023). What matters is not when running starts, but how prepared the knee is to absorb and recycle force.
Running introduces:
- Repetitive vertical loading
- Asymmetrical ground reaction forces
- Fatigue-driven changes in mechanics
If the knee cannot tolerate these loads symmetrically, running does not “build tolerance.” It reveals deficits.
This is why criteria such as quadriceps strength symmetry, absence of effusion, and controlled single-leg hopping are emphasized before progressing volume (Kotsifaki, 2023). Without those prerequisites, running becomes rehearsed compensation.

Phase 4: Plyometrics and Deceleration Are Where Rehab Gets Honest
Elite sport is not slow. It is fast, reactive, and chaotic. Most ACL injuries occur during deceleration, cutting, or landing, not during controlled strength tasks. Yet these qualities are often under-dosed or delayed until the final weeks of rehab, if they appear at all.
The Aspetar guideline supports the integration of plyometric and agility training in advanced rehab phases, noting improvements in functional outcomes without increased laxity or pain (Kotsifaki, 2023). Importantly, eccentric and plyometric training together appear more effective than either in isolation.
From the professional soccer data, persistent neuromuscular inefficiencies during high-speed actions remain common even after return to play (D’Ambrosi, 2025). This suggests that clearance often occurs before athletes are fully exposed to the demands that caused the injury in the first place.
Avoiding these demands in rehab does not make athletes safer. It simply delays exposure until the stakes are higher.
Phase 5: Psychological Readiness Is Not a Soft Skill
One of the most consistent findings across ACL research is also one of the least systematically addressed: psychological readiness matters.
Fear of reinjury, hesitation during cutting, and reduced confidence alter movement patterns in ways that increase joint loading. These factors do not resolve spontaneously with time (D’Ambrosi, 2025).
The Aspetar guideline explicitly includes psychological readiness measures, such as the ACL-RSI, within discharge criteria (Kotsifaki, 2023). This is not an academic exercise. Athletes who feel unprepared move differently, even when strength and mechanics appear adequate in controlled settings.
Psychological readiness is not about motivation. It is about exposure. Confidence grows when athletes repeatedly succeed in progressively demanding tasks. Rehab programs that avoid uncertainty deprive athletes of that learning process.
Why Rehab Must Extend Beyond “Clearance”
One of the most important insights from modern research is that rehab completion is not the same as return to competition.
The Aspetar guideline describes return to sport as a transition, not an endpoint (Kotsifaki, 2023). Clearance allows athletes to rejoin training. It does not guarantee readiness for competition intensity, volume, or unpredictability.
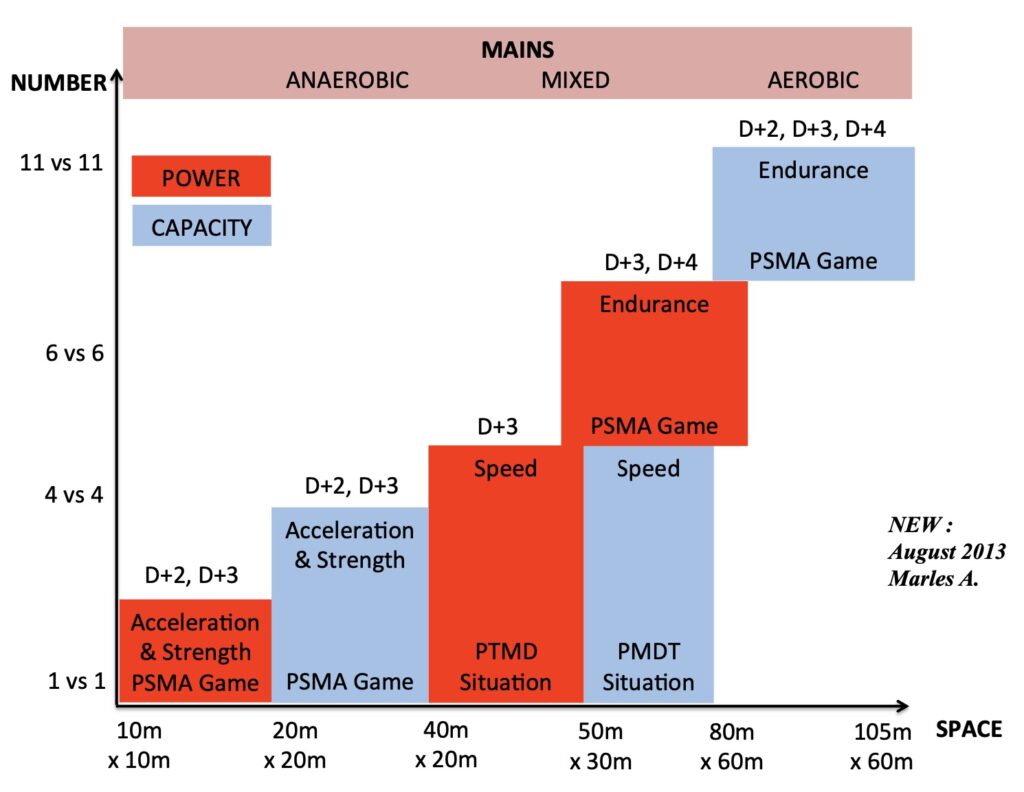
The professional soccer data reinforces this. Even with high return-to-play rates, reinjuries cluster after return, not during rehab (D’Ambrosi, 2025). That timing tells us the problem is not early exposure, but insufficient late exposure.
The Core Principle of Modern ACL Rehab Programming
When you strip away the protocols, timelines, and testing batteries, modern ACL rehab programming rests on one principle:
The knee must experience, and adapt to, the same stresses that caused the injury—before the athlete returns to sport.
Want a FREE Cheat Sheet for ACL Return to Play Criteria? check out my 360 Profile!
Watch More Like This
Related Podcasts
References
D’Ambrosi R, et al. Slower but Not Safer: A Systematic Review and Meta-Analysis of Return to Play and Graft Re-Rupture After ACL Reconstruction in Professional Soccer Players. Sports Medicine – Open. 2025.
Kotsifaki R, et al. Is 9 Months the Sweet Spot for Male Athletes to Return to Sport After ACL Reconstruction? Br J Sports Med. 2025;59:667–675.
Kotsifaki R, et al. Aspetar Clinical Practice Guideline on Rehabilitation After ACL Reconstruction. Br J Sports Med. 2023;57:500–514.




